Part One: Questionable Care & Insurance Denials
This is part one of my episodic retelling of battles fought, questions asked, and lessons learned this calendar year or in other words, six months post-transplant to present.
I fought insurance, my employer, my care team, and time.
I write from an extreme place of privilege. Acknowledging that, I never want people who stumble upon my blog to feel they are less entitled, less worthy, less able to fight. But if they do feel that way, I want it known that is precisely why I do fight — for them. I fight for those without a voice, a safety net, or a platform. I am highly confrontational. I am educated. I am articulate. I am a white woman. I have an above average health literacy given my access and my profession. I do not take this position lightly.
With my privilege, comes responsibility and I feel that every day. It’s why I am chair of our employee resource group for individuals with disabilities. It is why I tell my story to make people care. It’s why I demand time and take up space.
I have a loud voice, and I will be heard.
This year began with a shingles diagnosis, three subsequent hospital admissions at Cleveland Clinic’s main campus; all with the end goal to get me into an acute rehab facility. I was a draw on the healthcare system, taking up a bed, because I had to follow the formula to get insurance coverage for rehab despite the fact that I didn’t require the around the clock care of the hospital. I was instructed by my lovely and trusted MS team, that these were the hurdles I had to metaphorically jump through.
Even with their expert guidance and my direct access to my team, I did not fit a mold, a formula, a care path. I was both a medical and insurance anomaly. Therefore, I was denied.
I suffered — physically, emotionally, mentally and financially. I used precious energy to fight. I played insurance’s stupid, meaningless game that has a human cost. I wrote letters, called every number, sent emails, documented my life, and fought. Make no mistake, insurance is a game and there are winners and losers.
I hope, if one person reads this, they learn my formula for winning. I hope they feel empowered to fight back, to speak up.
The Battlefield
In February, I went to the emergency department with excruciating pain. I was admitted to the hospital and after a few days, shingles emerged meaning I at last had a diagnosis. You can read my words, mental state, and frustrations from that time.
Lesson one: Pain is still not taken seriously, especially for women.
Was I exaggerating? Faking? Hysterical?
They questioned the validity of my suffering.
Condescending in-patient neurological teams asked if the Tylenol was working. We won’t give you opioids, but we will use your body as a teaching vessel, a live person where medical students can play operation and experiment rather than help.
I was told they could stick needles into my neck and nerves. It might help; let’s try it. But no opioids, heaven forbid. I calmly informed them that the longer I was kept in distress, the worse my MS symptoms and janky nervous system would get. There would be physical ramifications. But what do I know? I’m not a doctor, I have no medical training. I couldn’t possibly know my body in the face of adversity better than them. My advocacy, my words, did nothing.
I screamed. I cried. I yelled. All decorum gone. My mom, seated by my bed, struck silent in the face of my outbursts. Then, miraculously, my pain was instantaneously validated with a diagnosis when previously it was dismissed. Shingles meant I was in fact telling the truth and I could now have opioids to help manage my pain. Shortly after administration, the comically benevolent doctors wanted to know if the opioids were helping. How was I doing? Were they kidding? It’s amazing how fast a medical team can lose the trust of a patient. It’s gone in the blink of an eye. I was discharged home. I was able to work, and friends watched me like babysitting shifts. My walking declined; paralysis was taking over as my body is wont to do. I went back to the hospital for the second time.
This admission, I was placed in a single room in the J building, aka the Ritz Carlton of Cleveland Clinic’s main campus.
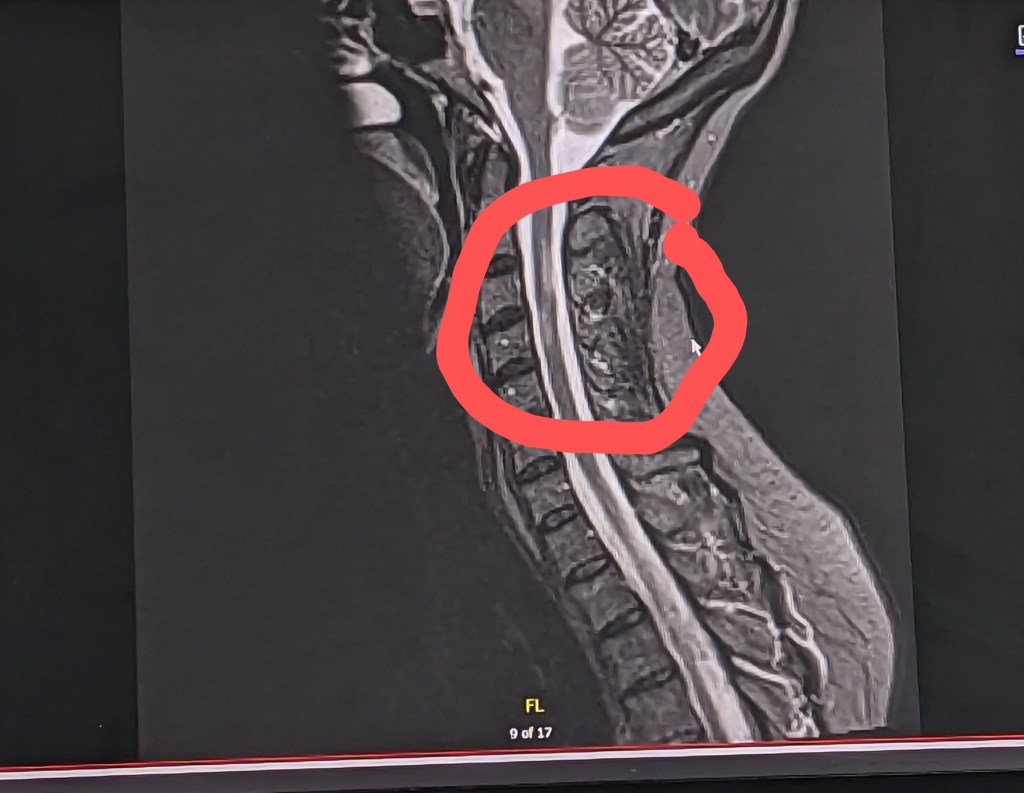
Another new in-patient neurologist looked at my MRI films and loudly stated, “Wow, with all those lesions on your cervical spine, I’m amazed you can walk at all.” I replied back, “Wow, what a supremely unhelpful and hurtful thing to say!” He was appropriately apologetic at his outburst. I suggested he think before he speak next time because his words were incredibly damaging to my tenuous hope and mental stability.
Lesson two: Know the ‘why’ behind the question they are asking.
And, answer appropriately.
They asked if I had a safe place to go, I answered yes. I was discharged to my parents. I’m lucky, I have generous parents with a one-story home who are retired and could help. I answered incorrectly because we weren’t speaking the same language. My goal was to live independently. My goal was to be self-sufficient, to work, to take care of myself. I needed a safe place to recover and actively rebuild my lost mobility. So, I did have a safe place to go, but that’s not the same thing.
While at my parents, I collapsed on their bathroom floor. I saw a pain specialist; I still couldn’t walk. I wasn’t sleeping and I was hoarding my precious opioids because I was well aware of the battle to get the meager allotment and uninterested in trying to get more. I didn’t have it in me to fight. I needed help, skilled rehab to retrain my frazzled nerves in the subtle art of walking. I needed occupational therapy assistance. Back to the hospital I went for the third time.
Lesson three: All doctors, residents and nurses are not created equal.
Ask questions, demand their time, attention and care.
Have impossibly high standards.
I endured questionable care, dismissive doctors, traveling nurses, and hospital coffee as I waited. One traveling nurse asked me one morning when he came on shift what I did to deserve getting a hospital bed on the shit floor? The implication that I was at fault, like being sent to the principal’s office or prison. Compared to my room in the J building, I was in a shit room, but the hospital room does not determine the level of care or attention received. He didn’t know I worked there obviously, but regardless of my employer, how many other patients did he say that to?
I had a consult with PM&R (physical medicine and rehabilitation). Insurance required their consult and opinion for pre-approval for the desired acute rehab facility. The young PM&R resident didn’t even bother with a physical examination. He assured me, with little knowledge of my case and zero knowledge of HSCT, that I would be denied, and I was wasting my time.
I am not a forgone conclusion for anyone, least of all a doctor I am meeting for the first time and interacting with for less than 10 minutes. I took out my work phone and took a photo of his ID badge. I texted it to my neurologist’s fellow in front of the jerk PM&R resident. He asked what I was doing, and I told him without artifice, that I was ensuring he wouldn’t touch my case going forward. I was essentially, firing him.
I told the attending neurologist and neurological team that he was a rude, dismissive, and horrendous doctor when they inquired about my PM&R consult. I asked that his notes in my medical record be expunged; I deserved another PM&R consult. Someone listened because that awful resident’s supervisor and attending physician visited me later in the day, did in fact administer a neurological exam, and apologized for the care I previously received. Again, my mom bore witness to it all.
My entire neurological team, the new in-patient attending and team on service as well as my long-standing MS doctor, agreed the acute skilled rehab facility was the best place for me. Insurance approval was submitted and denied. They went back and argued and fought for me with more information, paperwork, phone calls. It was denied a second time. My medical team continued to fight, to call, to advocate. I wasn’t consulted or questioned by insurance or medical review committees. And despite the fact that their decisions were about me, I had no part to play. My fate was in their hands. I had to wait over the weekend — in the hospital — for the appeal. I wrote one of my favorite posts during that time about the versions of me I mourn.
I was denied by insurance a final time.
Economic Privilege
Mentally and emotionally exhausted and physically battered and bruised, we asked what it would cost to pay out-of-pocket. One week in skilled rehab was $10,000.
We paid it.
Even in the 11th hour with my discharge imminent, my inpatient neurologist said I could go to a skilled nursing facility or SNF (read SNIFF in medical speak). He admitted it was a less-good option, but it would probably be covered by insurance. He told me one hour of rehab was better than nothing. Was I sure I wanted to pay out of pocket?
I knew what I needed to get better. I had my mother and father cheering me on and making this decision a possibility. I knew that I was capable of being pushed and could handle the three hours of OT and PT each day but that I also deserved to be safe. I had been paralyzed before; I knew I could come back from it with the right help. I was also willing to work hard, endure pain, and try. I had already wasted enough time on the insurance game. Time is a precious commodity.
How hard would you try to be able to walk? To maintain your independence? I would venture a guess that the individuals in charge of approvals and denials have never been faced with that question. They live in an illusion of health and are playing with people’s lives. It’s not a game, but it feels like one.

None of that mattered. My experience or the uniqueness of my case; my advocacy did not matter. Despite there being little to no precedent for individuals recovering from HSCT as a treatment for MS, I didn’t fit their perfect, stupid, awful, non-human formula. Let me be abundantly clear: I have the gold standard of insurance. This is my experience with employer-subsidized, amazing insurance. And my words, despite my best efforts and every “phone a friend” favor I called in, were useless.
I was discharged and we paid $10,000 to get the care I knew I needed. I wrote about my week-long stay in rehab.
Lesson four: For the love of God, WRITE IT ALL DOWN!
As if the chronically ill need one more thing to do, you must keep track of everything. No one else is going to do this for you. Don’t trust the 5,000 medical professionals who will touch your case, round on you, administer meds, and offer advice to be the subject matter expert. It’s you! Write it down. Take photos with your smart phone. Use the notes app and leave voice memos. Record videos of your experience in the camera app. Take photos of badges. Ask questions. Be a pest.
A less emotional but still important example: I was in-patient the third time and the nurse came in with my nightly meds. She informed me it was time for my nightly heparin shot. I asked what the shot was for; why did I need a blood thinner? “Standard procedure” was said back to me as she prepared the needle. I said, “Please stop!” I wanted to understand the medical reasoning behind the blood thinner shot. “It’s to prevent blood clots,” she said. I told her I wasn’t at risk for blood clots and was sitting up in bed, stretching, manually moving my legs and more. With difficulty, I was still walking to and from the bathroom. I wasn’t at risk for blood clots, was I? I used my favorite phrase, “help me understand.” If there was a medical reason for the drug, I would have taken it, but I asked in order to know and more importantly to understand the medical reasoning, and that is my inherent right.
Long story short, there wasn’t a reason for me to take it beyond hospital protocol. I declined the shot. That denial was documented in my medical record, and I had the EXACT SAME CONVERSATION each consecutive night with each new nurse as I declined the shot for the rest of my stay.
Because I write things down, I had a record not only of my emotional and physical state but the who, the what, the when, and the how many times I interacted with people, had conversations, challenged my care, and was told conflicting information. When I was concerned that I misremembered something, I called upon my friends and family who witnessed the majority of these conversations.
All this information would come into play down the road as I went to battle with insurance and used precious energy to personally appeal. I took back my story, found my voice yet again, and relied on all documentation to get to the bottom of my insurance denial.
Unforeseen Consequences
Part one of this story made me less sure about the whole HSCT process, my ongoing care and treatment, and my path forward. It made me question my ability to heal, the hard-won hope I had gained. I became mistrusting of doctors and the advice they gave. I was broken hearted that it was ok to experiment on me in the name of medicine and science, but there was no assurance of aftercare. I could pay for the care I needed, but could others? How would they manage in the face of so much adversity?
I felt utterly alone and abandoned by medicine. Honestly, months later, I still feel the effects of that time. A proponent of research from the start, when called recently to schedule my follow-up 7T MRI, I declined. I was unapologetic in my refusal. I was not willing to undergo the discomfort, pain, anxiety and apprehension for them. The research assistant was lovely and understanding. Still, I feel like I failed my fellow MS’ers somehow. But no way was I giving an ounce more of me than I already had.
It was the only card I had to play. I withdrew from the game.
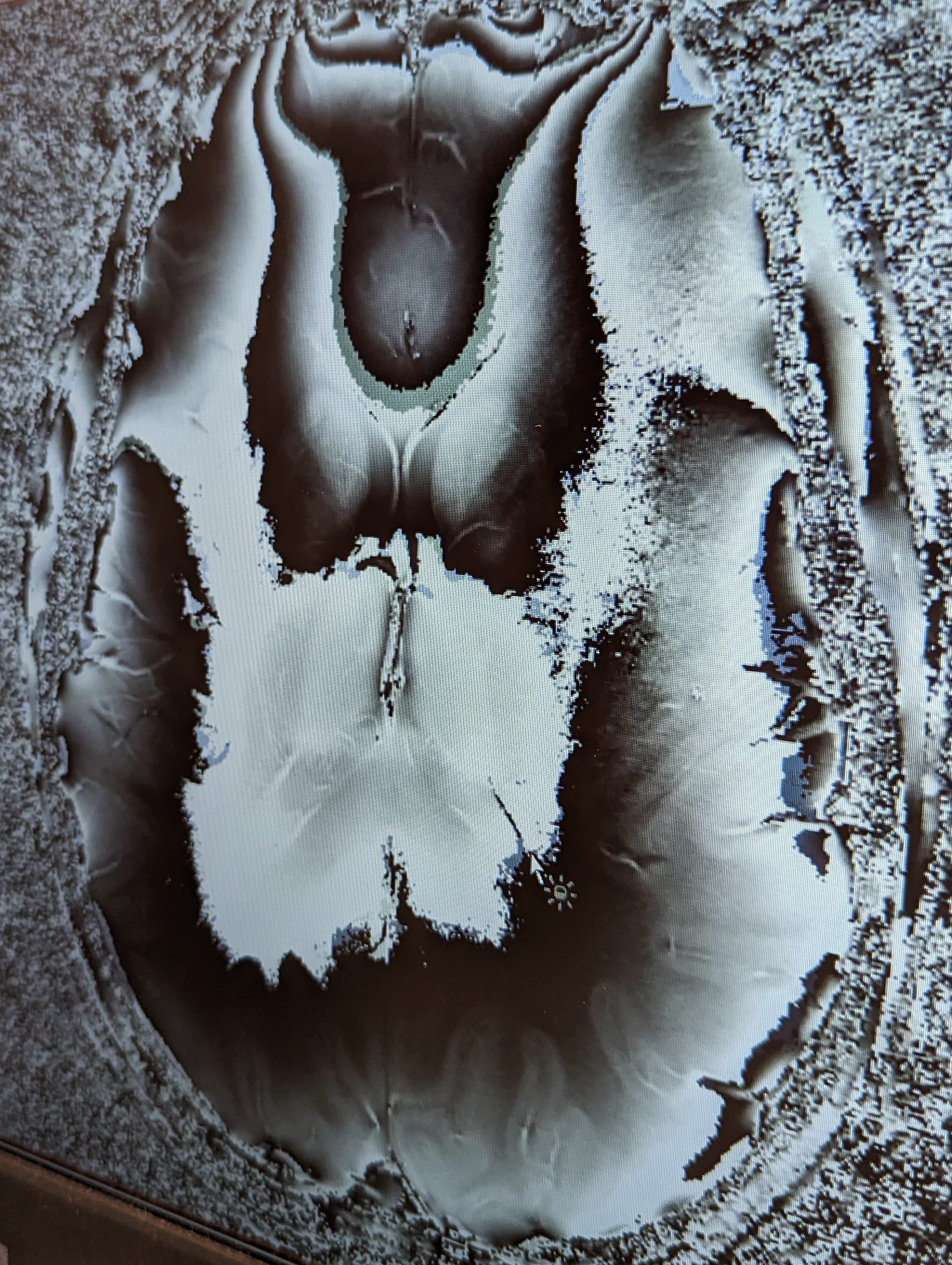
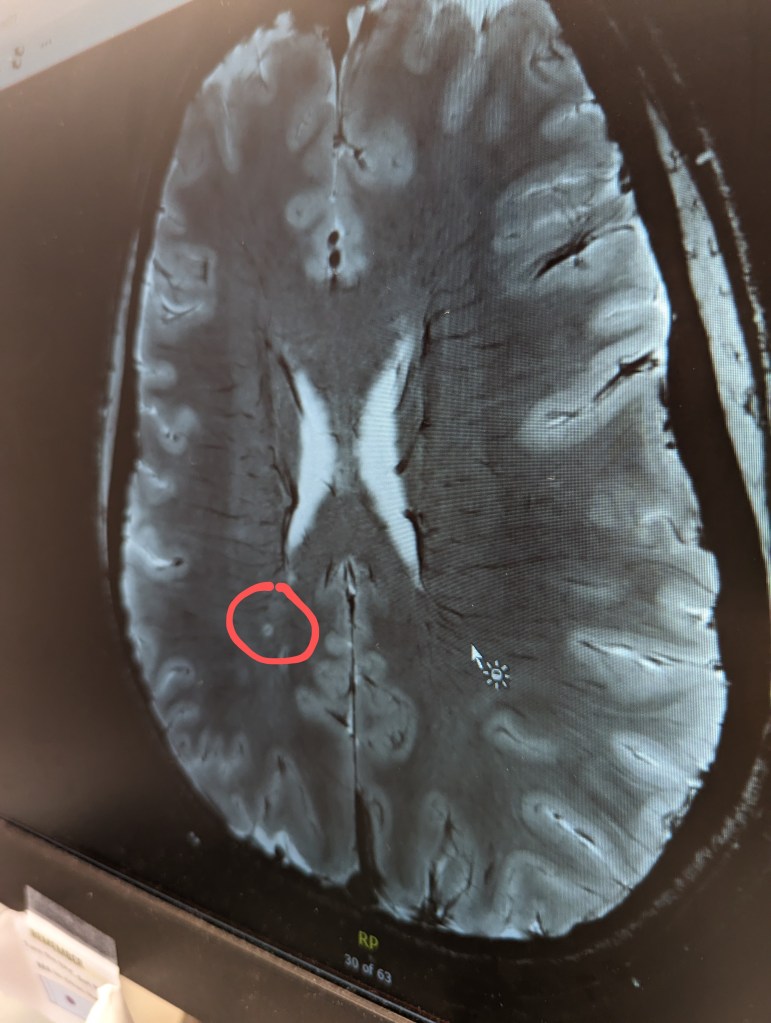
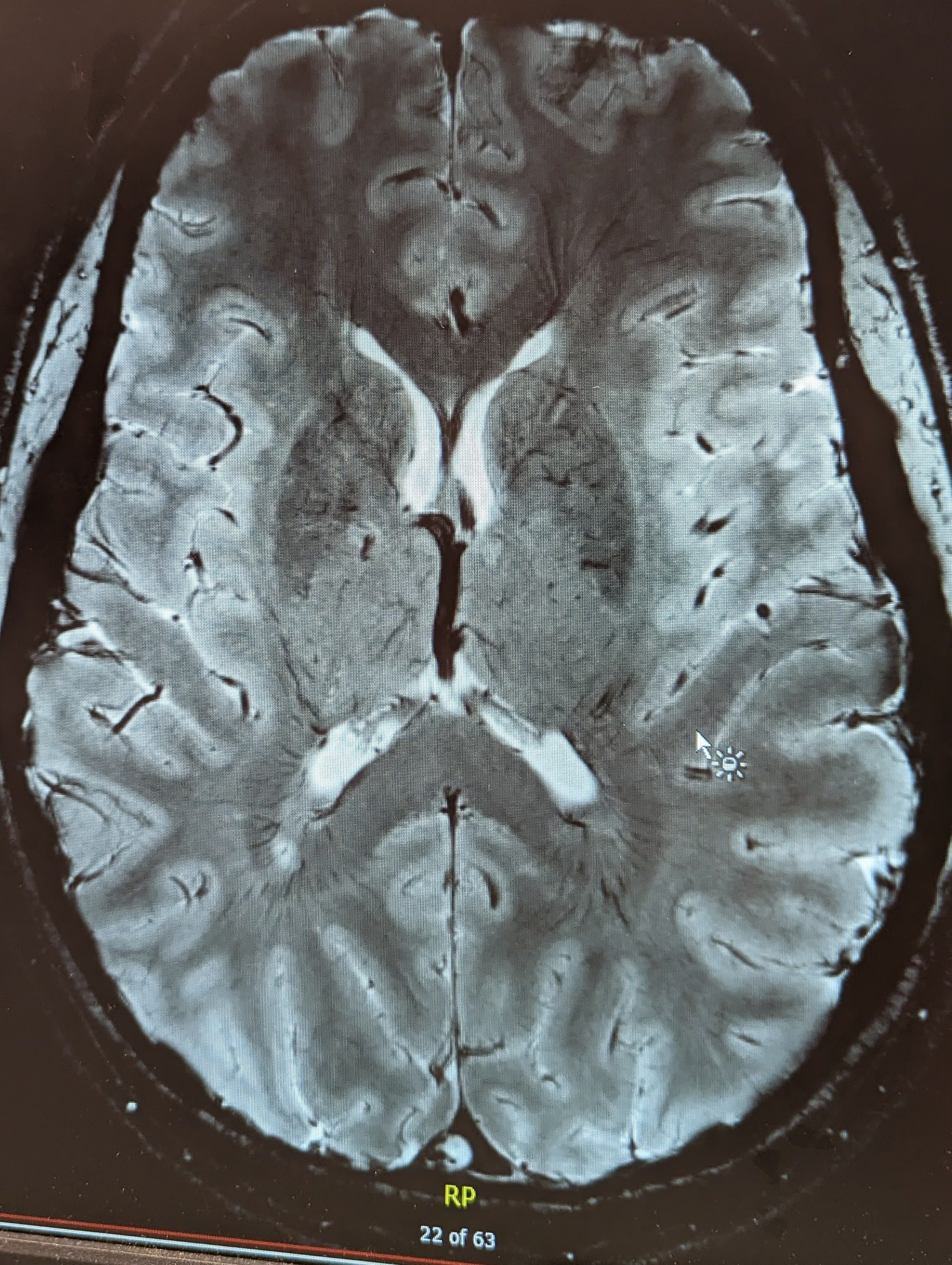
Images above are my brain. The red circle represents one of my very few brain lesions. The image on the left maps water movement throughout my brain.
To be continued


2 responses to “Speak Up: I will not go quietly into the night”
Carolyn, I just finished reading your latest blog entry. If I had been able to witness all that you described, but without having gotten to know you through your previous entries, I would have considered you a royal pain in the neck! Thank you once again for writing in such away as to open my eyes and my mind and know that I have learned something I NEED to know. This is not to say I expect to have a similar experience with my health and insurance, though I could, but what I keep learning is that there are areas in my life about which I have had a lifelong ignorance, simply because I have not been exposed to them. Fighting doggedly with my insurance company is one of those things.
Here’s another thing in which I have lived my whole life in ignorance: internalized racism. Have you ever heard of that? I came across it for the first time in the book, “Be the Bridge” by Jennie Allen, that I’m currently studying with a group. The author doesn’t provide a definition for it, but from the context I think it means a certain attitude or preconceived notion that is so ingrained we don’t identify it. Your words in paragraphs 3, 4, and 5 echo some of the same language, like “privilege” (white), “safety net” (assumed, but not a reality for most).
So thank you for the enlightenment. In fact, your retorts to your doctors and medical personnel made me smile and think to myself, “You go, girl! “ I can barely wait till your next entry!
LikeLike
I always appreciate your perspective and comments, Beverly. I think I can be both things that you mentioned at the same time. I am a pain in the neck. I am difficult. I wish I didn’t have to be. I still believe in my bones that the majority of medical professionals I interact with have the purest of intentions and want the best for me. Many of the people mentioned above worked their butts off to try and get insurance approvals. No one is confused on the doctor side or the patient side about the game of insurance. I’m so glad that I can present a different perspective for individuals in their own health interactions. As always, I appreciate you reading and the words that you share.
LikeLike